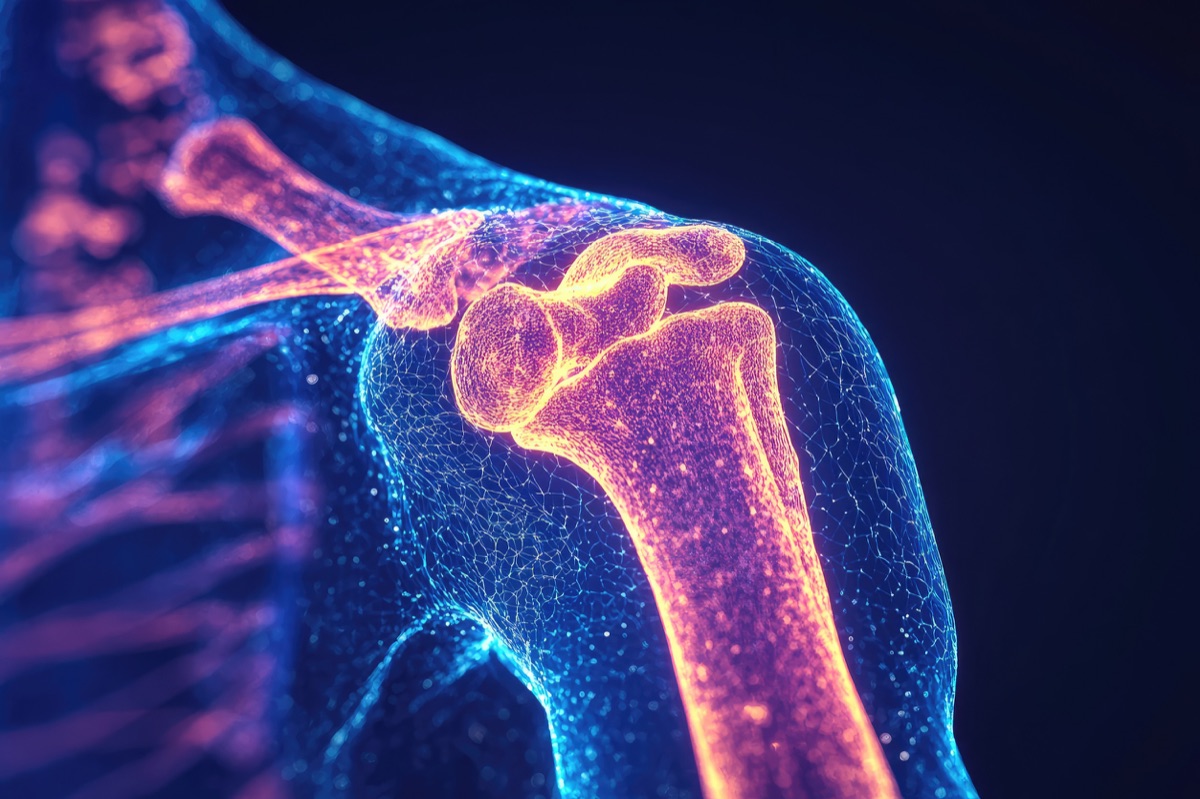
Shoulder Pain:
Complete Guide
The shoulder is the most mobile joint in your body—and that flexibility comes at a cost. Understanding the complex anatomy of your shoulder is key to finding relief and restoring function.