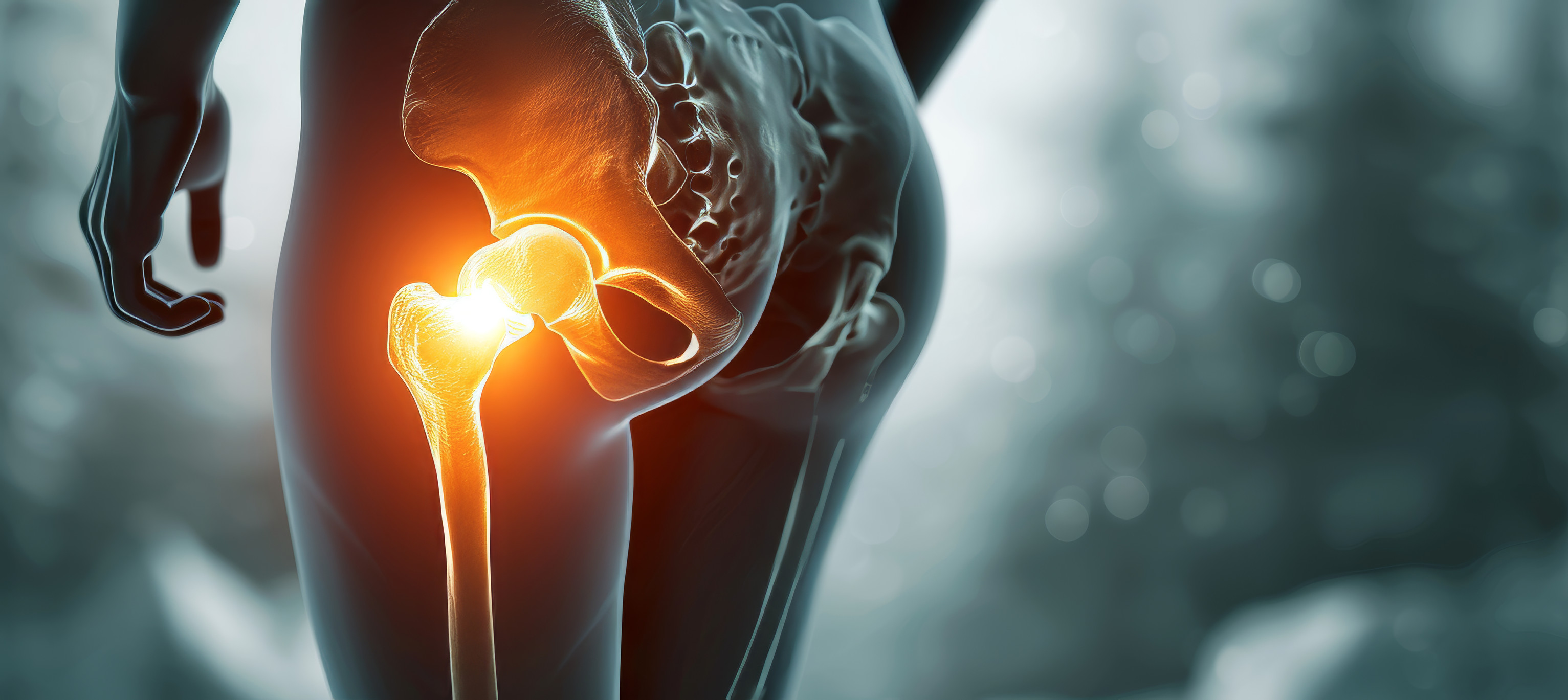
Hip Pain:
Complete Guide
The hip is a ball-and-socket joint designed for stability and a wide range of motion. When problems develop, hip pain can significantly impact your ability to walk, sit, and perform daily activities.