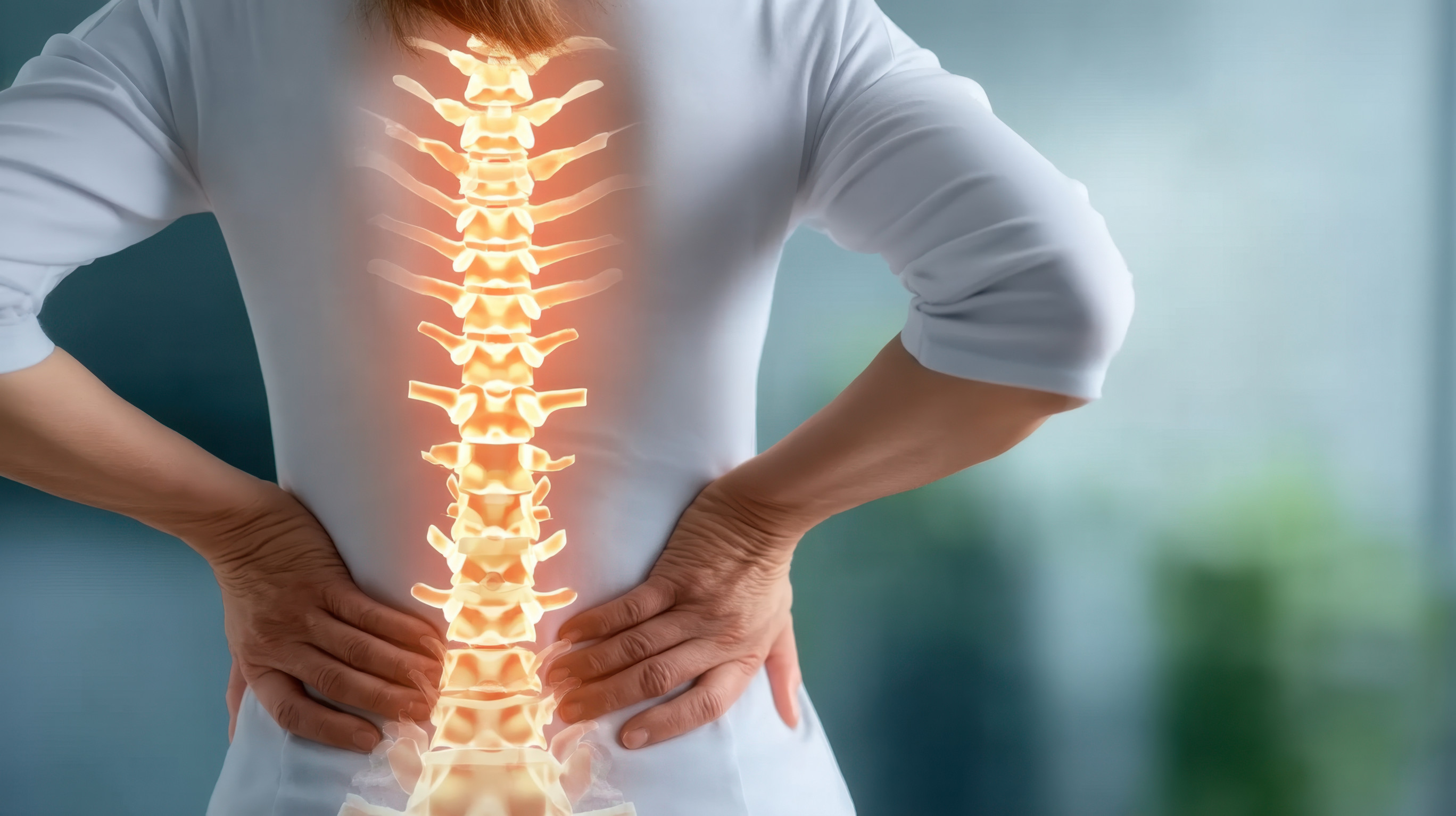
Back Pain:
Complete Guide
Back pain is one of the most common reasons people seek medical care. The spine is a complex structure of vertebrae, discs, nerves, and muscles—understanding your pain is the first step toward lasting relief.